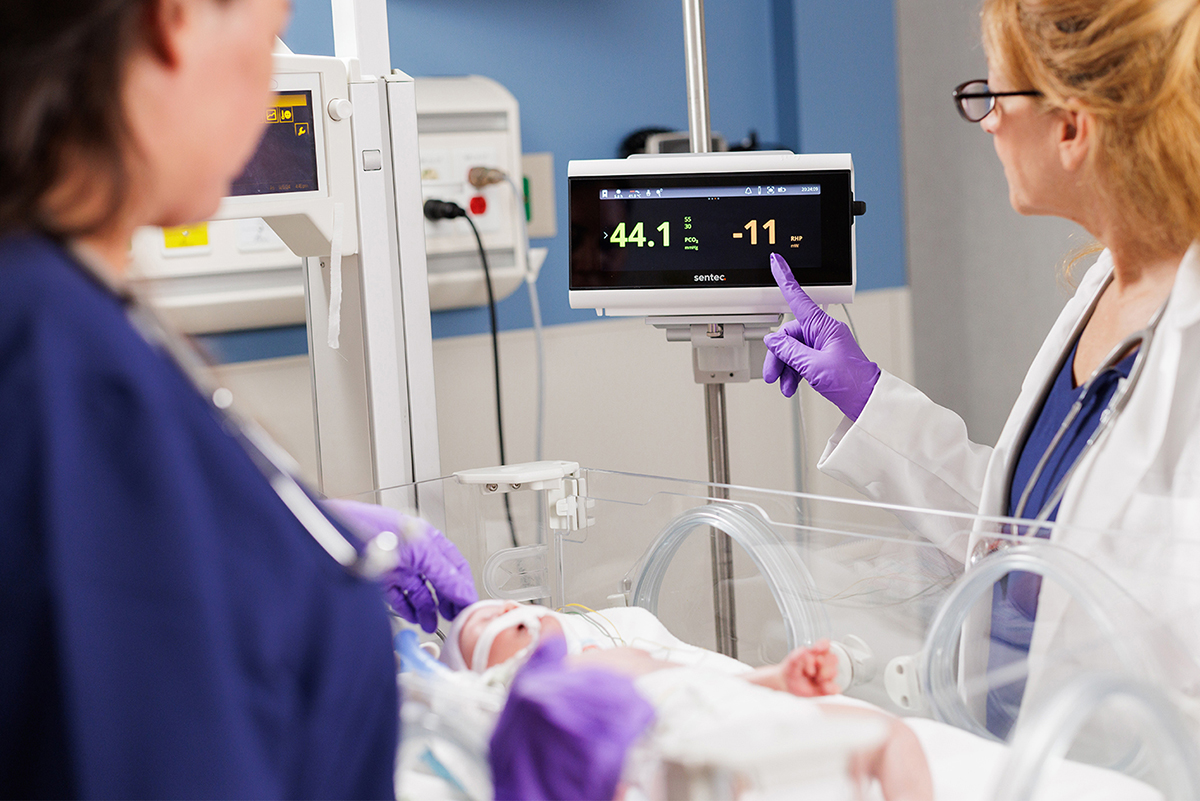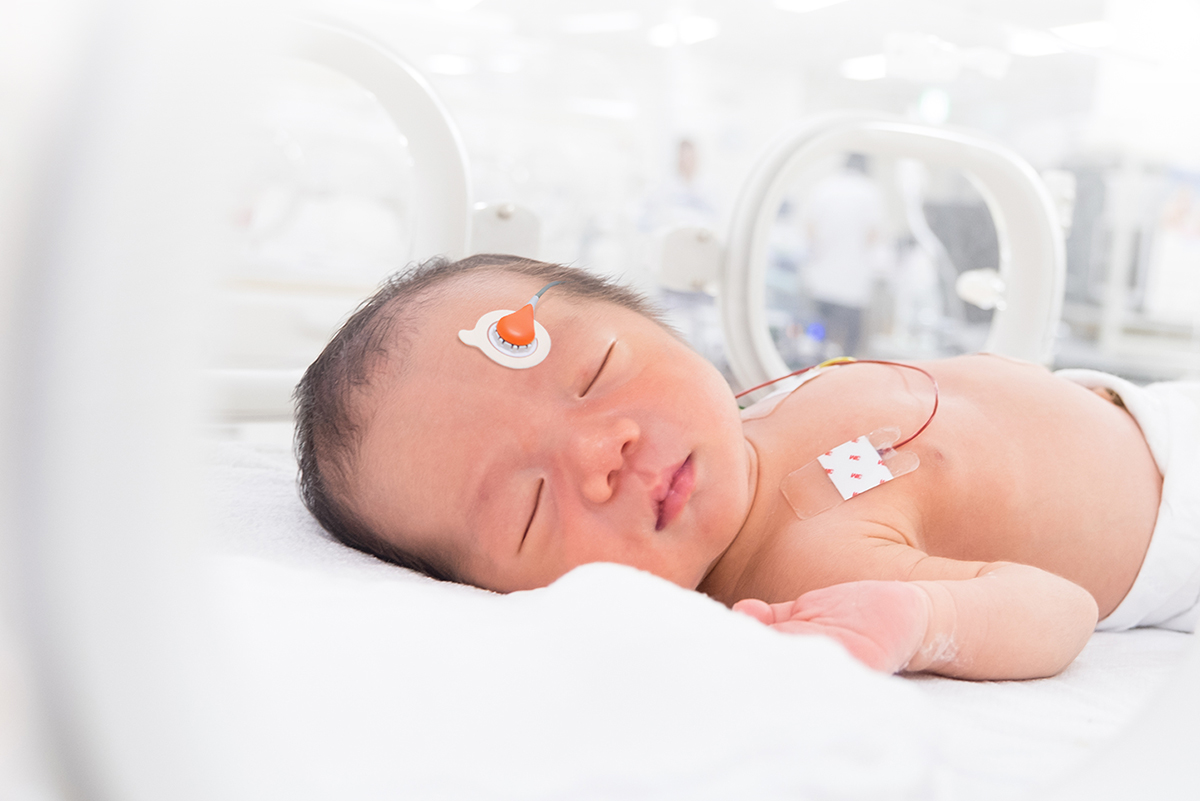
WHY CONTINUOUS MATTERS
Balancing Brain and Lung Protection
A core goal in the NICU is to protect infants from brain injuries like intraventricular hemorrhage (IVH) through careful management of ventilatory support. However, this support has inherent risks: delivering too little volume can lead to derecruitment and atelectasis, while too much can cause overdistension and volutrauma.
Continuous, accurate CO2 monitoring supports NICU teams in striking the right balance — providing enough respiratory support to protect the brain while remaining gentle enough to preserve fragile lungs.
NONINVASIVE MONITORING FOR LESS INVASIVE CARE
Reducing Pain and Blood Loss
Blood gases are checked frequently in the NICU, and for a tiny preterm baby, this sampling can quickly result in meaningful cumulative blood loss. More over, each heel stick or arterial sample causes pain and stress, which has shown negative impacts in neurodevelopment, such as:
- Lower Mental Development Index between 8 and 18 months¹
- Poorer visual-perceptual abilities at school-age²
- Reduced white matter and lower IQ at 7 years³
PROVEN IMPACT
From Implementation to Impact in the NICU
Adopting transcutaneous CO2 monitoring and standardizing its use across the NICU team has demonstrated outcomes that truly matter for the hospital’s tiniest patients.
Woman’s Hospital NICU | Baton Rouge, Louisiana
Achieved a 50% reduction in blood draws for extremely preterm infants within the first year of standardizing transcutaneous CO2 monitoring.4
Penn State Health Children’s Hospital NICU | Hershey, Pennsylvania
Minimized blood draw frequency from every four hours to every 12 hours after implementing transcutaneous CO2 monitoring.5
Children’s Hospital of Philadelphia NICU | Philadelphia, Pennsylvania
Reduced daily blood gas draws on ventilated patients by over 25% following the introduction of transcutaneous CO2 monitoring into the unit.6
University of Alabama at Birmingham NICU | Birmingham, Alabama
Reduced the mean rate of severe intracranial hemorrhage (ICH) or death in the first week after birth by more than 10% following the institution of a care bundle for neonates, which includes the use of transcutaneous monitoring to target safe CO2 levels.7
Benefits for Patients
Benefits for Providers
Benefits for Facilities
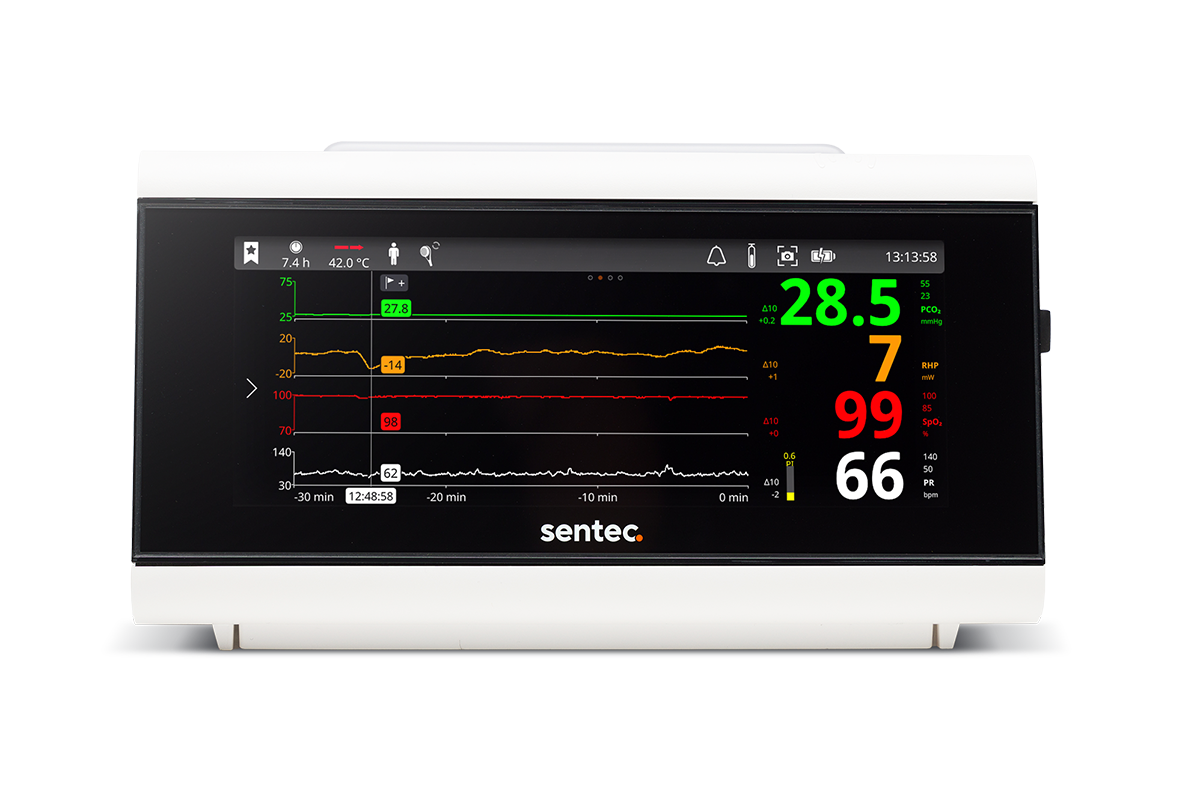
tCOM+
CO2 Monitoring Designed for the NICU
The Sentec tCOM+ is built with the NICU in mind, delivering the accuracy clinicians rely on to guide care, along with features tailored to the unit’s unique clinical and operational needs, such as:
- Smart Cal-Mem: Disconnect a patient for up to 30 minutes without recalibration, supporting kangaroo care and repositioning.
- Versatile attachment options: Includes a Non-Adhesive Wrap designed for VLBW infants in high-humidity environments.
- Real-time event logging: Track the impact of interventions.
Recommended by Professional Associations Worldwide
American Association of Respiratory Care | Clinical Practice Guideline8
Recommends transcutaneous CO2 monitoring “to determine the presence of hypoventilation or respiratory depression” in:
- Conventional modes of ventilation
- High frequency ventilation
- Steady state high frequency jet ventilation
- Noninvasive ventilation
- Transportation of a patient
- Bronchoscopies or procedures requiring sedation
- Prolonged laparoscopic surgery procedures
- Sleep studies
- Pulmonary function studies
- Evaluation of postoperative hypercarbia
- Titration of long-term oxygen therapy
Swiss Society of Neonatology | Standards for Levels of Neonatal Care9
Recognizes continuous transcutaneous pCO2 monitoring as a requirement for Level IIB and Level III NICUs.
German Joint Federal Committee | Quality Assurance Guideline for Premature and Full Term Infants10
Requires that four of the six beds designated for intensive therapy be equipped for transcutaneous pCO2.
Western Australia Child and Adolescent Health Services | Transcutaneous Carbon Dioxide Monitoring Guidelines11
Indicates continuous transcutaneous CO2 monitoring in the NICU for:
- Admissions requiring mechanical ventilation for the first four days
- Surgical infants during the first four hours post-op
- Surgical infants requiring postoperative respiratory support for the first 24 hours
- Infants with pneumothorax
- The first four hours following extubation
National Institute for Health and Care Excellence (NICE) | Respiratory Care Guidelines for Preterm Babies12
Recommends transcutaneous oxygen monitoring in invasively ventilated preterm babies.
References
- Grunau, R.E., et al. Neonatal Pain, Parenting Stress and Interaction, In Relation To Cognitive And Motor Development At 8 And 18 Months In Preterm Infants. Pain. 2009.
- Doesburg, S.M., et al. Neonatal Pain-Related Stress, Functional Cortical Activity and Visual-Perceptual Abilities In School-Age Children Born At Extremely Low Gestational Stage. Pain. 2013.
- Vinall, J., et al. Invasive Procedures In Preterm Children: Brain And Cognitive Development At School Age. Pediatrics. 2014.
- Schorr, M., et al. Reducing Pain in the NICU: A Quality Improvement Initiative at Woman’s Hospital. Neonatal Intensive Care. 2025.
- Donnelly, A., et al. Transcutaneous Monitoring in the NICU: Overcoming Challenges and Driving Consistent Implementation in an Academic Medical Center’s Level IV NICU. 2021.
- Mukhopadhyay, S., et al. Neonatal Transcutaneous Carbon Dioxide Monitoring – Effect on Clinical Management and Outcomes. Respir Care. 2016.
- Travers, C.P., et al. A Quality Improvement Bundle to Improve Outcomes in Extremely Preterm Infants in the First Week. Pediatrics. 2022.
- Restrepo, R.D., et al. AARC clinical practice guideline: transcutaneous monitoring of carbon dioxide and oxygen: 2012. Respir Care. 2012.
- Bassler, D. Standards for Levels of Neonatal Care in Switzerland. Swiss Society of Neonatology. 2019.
- Gemeinsamer Bundesausschuss. BAnz AT. 2020.
- Government of Western Australia Child and Adolescent Health Service. Guideline: Transcutaneous Carbon Dioxide Monitoring (TCM). 2006.
- National Institute for Health and Care Excellence. Specialist Neonatal Respiratory Care for Babies Born Preterm. 2019.
Still have questions?
Complete this form for additional product support. After you’ve submitted your query, the appropriate Sentec associate will reach out with more information.