
Understanding Ventilation Means Understanding CO2
The Role of Transcutaneous CO2 Monitoring
In today’s sleep lab, ventilation monitoring is essential—particularly for patients with complex respiratory physiology.
Transcutaneous CO2 monitoring (tcpCO2) offers a noninvasive, continuous estimation of arterial CO2 that:
- Enables uninterrupted CO2 trending throughout split-night studies
- Delivers accurate values even in the presence of V/Q mismatch
- Reduces reliance on potentially misleading surrogates like SpO2 and etCO2
With Sentec’s tCOM+, your team gains access to a versatile monitoring solution designed specifically for the realities of sleep care.
V/Q Mismatch
When End-Tidal CO2 Falls Short
While capnography has long been used in respiratory care, it presents well-documented limitations in the sleep lab environment—particularly in patients with impaired gas exchange.
End-tidal CO2 (etCO2) may be inaccurate due to:
- Ventilation/perfusion mismatch (common in COPD, asthma, OHS, and neuromuscular disorders)
- Gas mixing and dilution from NIV devices
- Interface changes during split-night studies
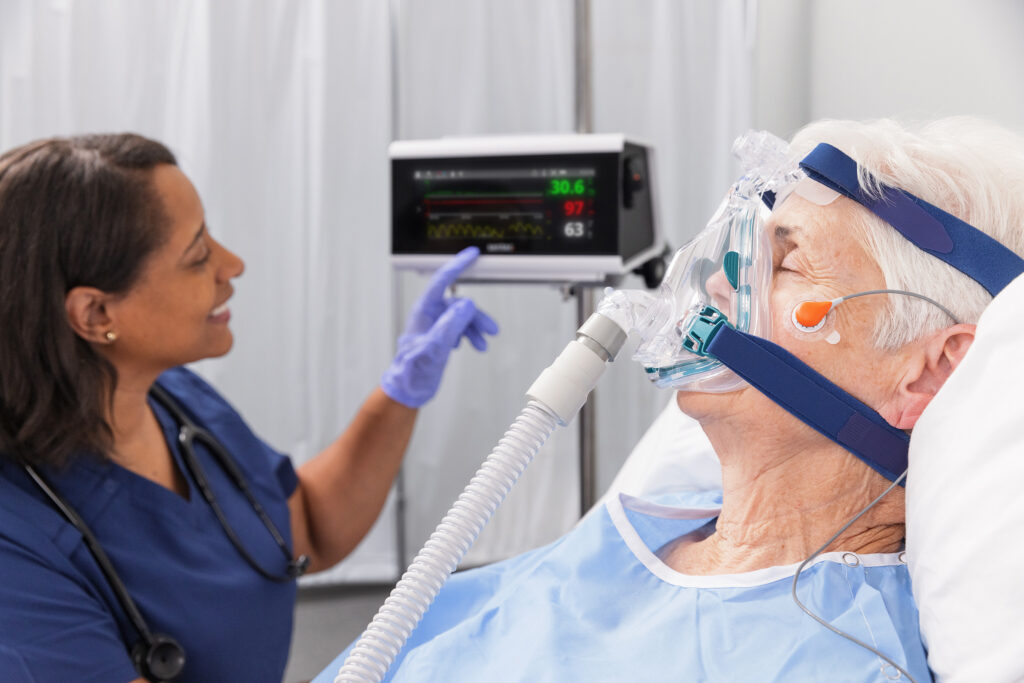

V/Q Mismatch
When End-Tidal CO2 Falls Short
While capnography has long been used in respiratory care, it presents well-documented limitations in the sleep lab environment—particularly in patients with impaired gas exchange.
End-tidal CO2 (etCO2) may be inaccurate due to:
- Ventilation/perfusion mismatch (common in COPD, asthma, OHS, and neuromuscular disorders)
- Gas mixing and dilution from NIV devices
- Interface changes during split-night studies
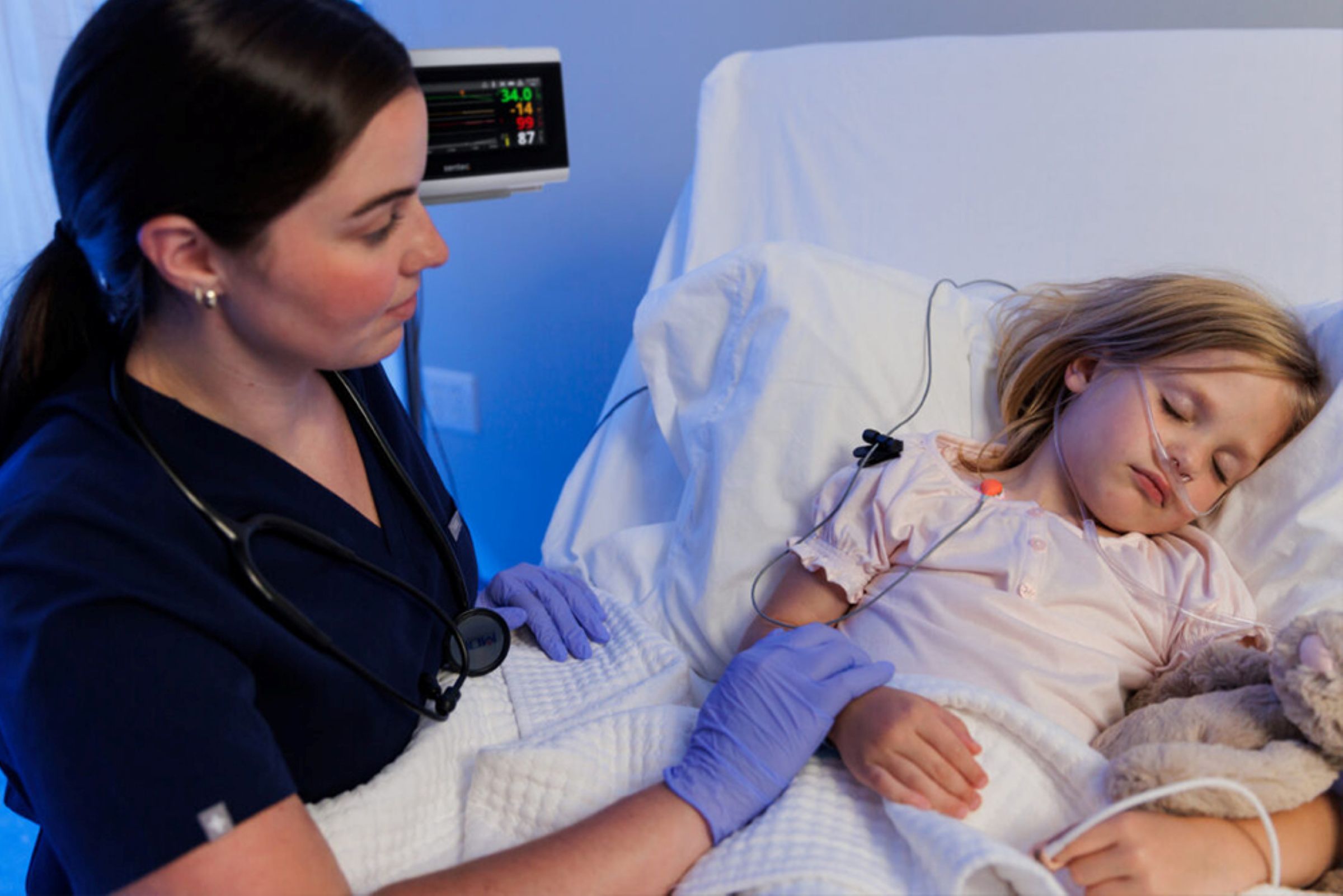
DESIGNED for the Sleep Lab
Monitor CO2 accurately, throughout the night
The Sentec tCOM+ is purposefully engineered to support the sleep lab's clinical and operational needs. Smart Cal-Mem™ allows up to 30 minutes of disconnection without recalibration—supporting patient comfort without sacrificing data integrity.
Key benefits include:
- Continuous, uninterrupted monitoring across therapy transitions and split-night protocols
- 12-hour site times and 28-day membrane life for efficient overnight use
- Seamless PSG integration, transmitting only stabilized data to reduce artifact and streamline interpretation
Trusted by Sleep and respiratory institutions
Backed by Professional Associations and Used in Sleep Labs Worldwide
Sentec’s transcutaneous technology aligns with recommendations from leading sleep and respiratory organizations. The American Association of Sleep Technologists (AAST) recommends using arterial or transcutaneous CO₂ measurement during PAP titration, while the American Association for Respiratory Care (AARC) recognizes the growing role of tcpCO2 monitoring in detecting sleep-related hypoventilation and evaluating therapy effectiveness.
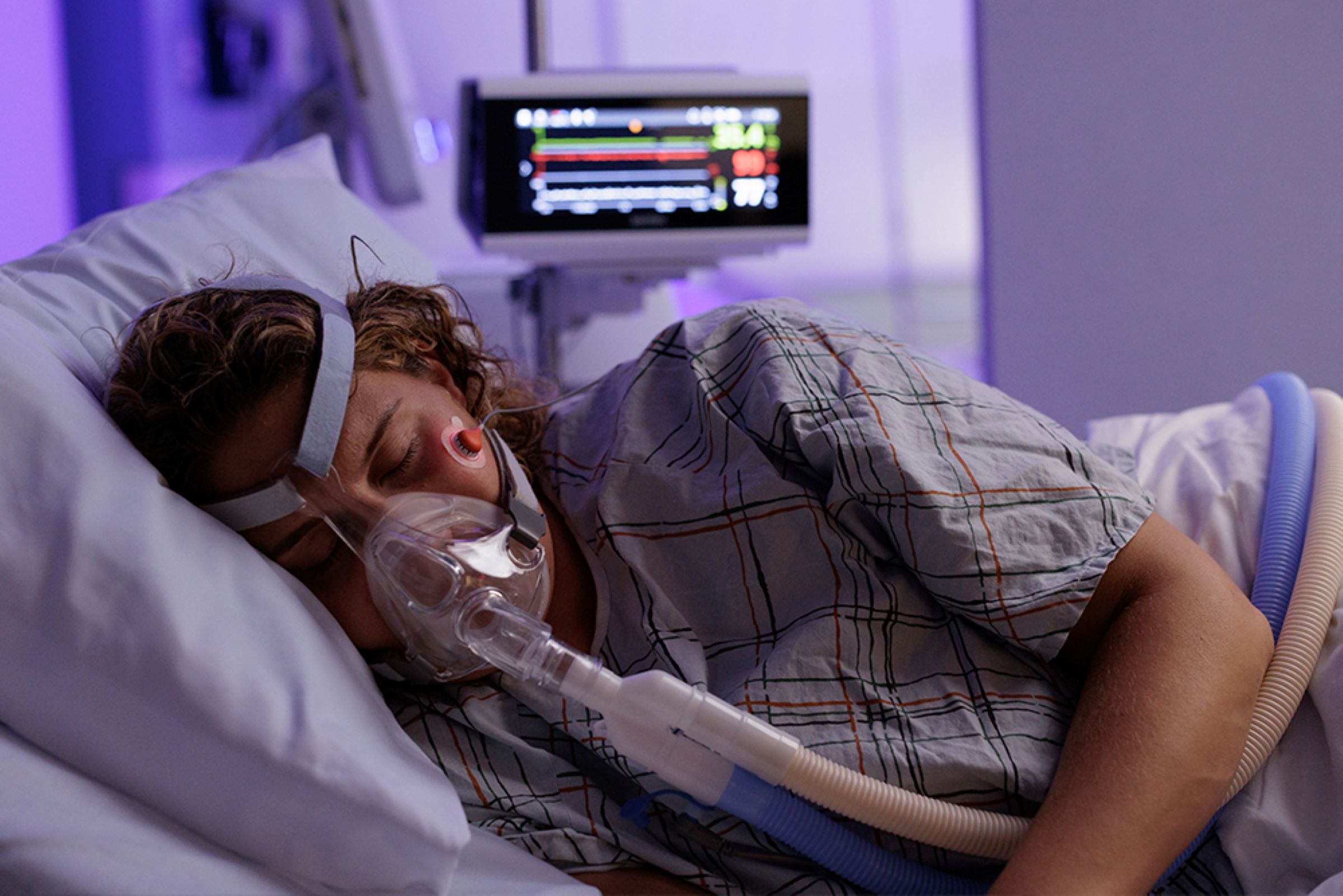

Trusted by Sleep and respiratory institutions
Backed by Professional Associations and Used in Sleep Labs Worldwide
Sentec’s transcutaneous technology aligns with recommendations from leading sleep and respiratory organizations. The American Association of Sleep Technologists (AAST) recommends using arterial or transcutaneous CO2 measurement during PAP titration, while the American Association for Respiratory Care (AARC) recognizes the growing role of tcpCO2 monitoring in detecting sleep-related hypoventilation and evaluating therapy effectiveness.

Case Studies with transcutaneous monitoring
Transcutaneous CO2 Monitoring in Routine and Advanced Pediatric Sleep Studies
“Transcutaneous CO2 monitoring can support sleep lab teams in overcoming challenges like mouth breathing, secretions, compliance issues, and the dilution effect from oxygen supplementation and PAP therapy, which may limit the effectiveness of end-tidal monitoring.”
– Lisa DeGuzman, RRT-NPS, RPSGT, CCSH
Pediatric Sleep Center & Pulmonary Function Test (PFT) Lab Manager at Nemours Children’s Hospital in Orlando, Florida
Get Transcutaneous CO2 Monitoring in Your Sleep Lab
Start the conversation about how our solutions can fit into your practice and support your care goals.

