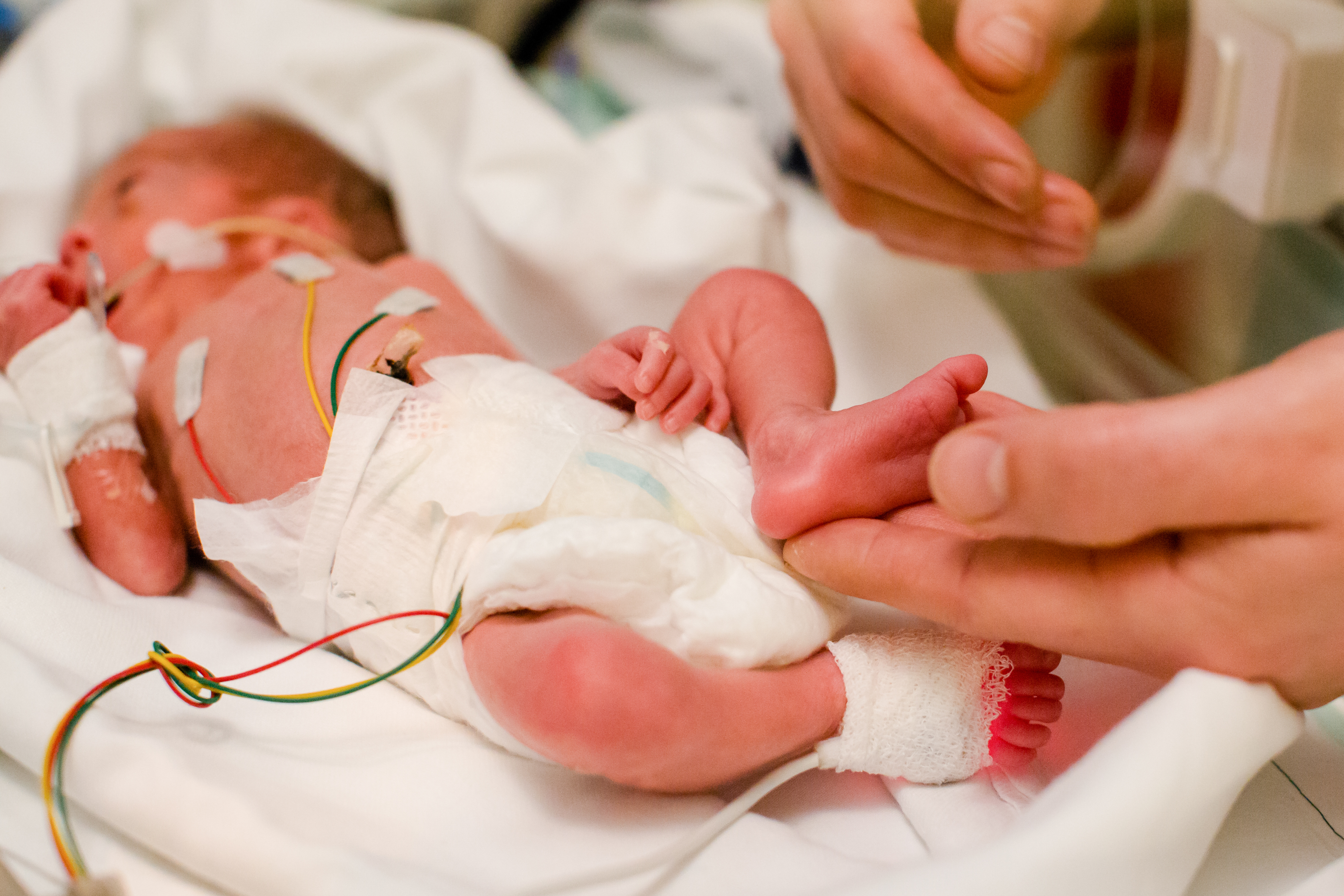
The Difficulties and Tradeoffs of Caring for the Most Fragile Patients
Providing the best care for the most fragile NICU patients is full of challenges and tradeoffs. Sometimes the information doctors need to gather from their patients comes at a cost. When neonatal care teams need to assess how a patient is responding to the current level of ventilatory support, a blood draw is traditionally required. However, that blood draw can contribute to blood loss, pain, and infection risk for the infant.
Why do we need to ventilate NICU patients?
Caring for preterm infants requires 1) ventilating their underdeveloped lungs and 2) protecting their brains—which often have immature blood flow regulation—from intraventricular hemorrhage and other complications.
To determine whether or not the ventilation support that these patients are receiving is adequate, clinicians need to frequently measure and monitor the amount of indicative substances in the blood. One of the most critical is carbon dioxide (CO2).
To read the complete whitepaper, fill out the form on this page.
To download the whitepaper, please fill out the form below: