Summary:
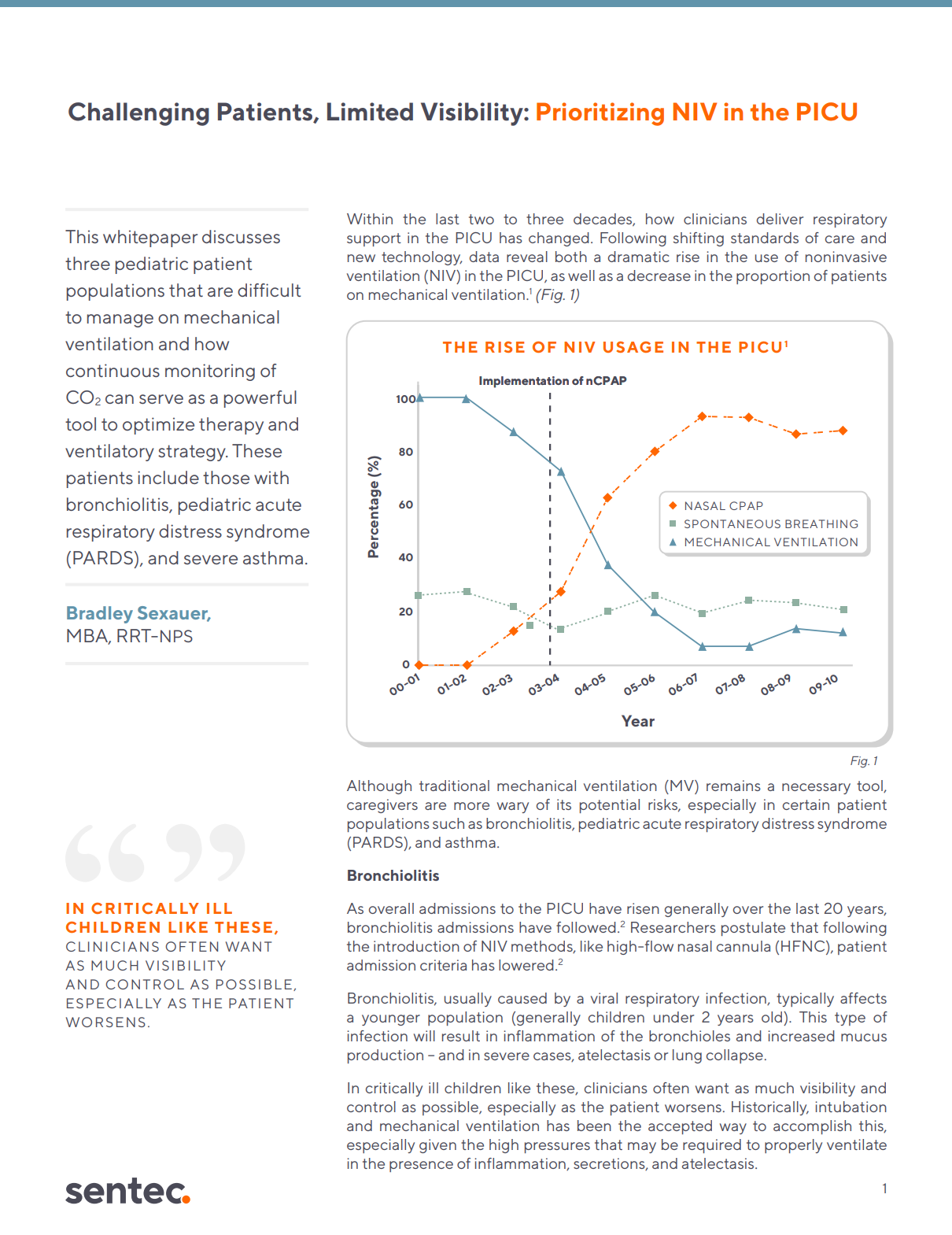
Within the last two to three decades, how clinicians deliver respiratory support in the PICU has changed. Although traditional mechanical ventilation (MV) remains a necessary tool, caregivers are more wary of its potential risks. This whitepaper discusses three pediatric patient populations that are difficult to manage on mechanical ventilation and how continuous monitoring of CO2 can serve as a powerful tool to support noninvasive ventilation (NIV) strategies and therapies in the PICU. These patients include those with bronchiolitis, pediatric acute respiratory distress syndrome (PARDS), and severe asthma.
Preview:
Is NIV the answer?
While mechanical ventilation and intubation is often necessary for the sickest, most compromised patients, NIV offers some advantages, especially in these patient populations. For children who are still able to breathe spontaneously, NIV modalities like HFNC allow them to continue breathing on their own schedule with added support, avoiding the issue of ventilator asynchrony and preserving respiratory strength ideally to either delay intubation or prevent it altogether.
Support Strategies and CO2 Visibility
The drawbacks of NIV come back to the control of and visibility into patient status, as discussed above.
Across ventilation modalities, from supplemental oxygen to intubation, clinicians have access to vital signs like SpO2, pulse and respiratory rates, and patient work of breathing. However, visibility to other important parameters (and tools utilized to get it) can vary, depending on how the patient is supported. CO2 is one of these critical values. CO2 monitoring is integral to understanding how well or poorly a patient is ventilating, particularly because…
Summary:
Within the last two to three decades, how clinicians deliver respiratory support in the PICU has changed. Although traditional mechanical ventilation (MV) remains a necessary tool, caregivers are more wary of its potential risks. This whitepaper discusses three pediatric patient populations that are difficult to manage on mechanical ventilation and how continuous monitoring of CO2 can serve as a powerful tool to support noninvasive ventilation (NIV) strategies and therapies in the PICU. These patients include those with bronchiolitis, pediatric acute respiratory distress syndrome (PARDS), and severe asthma.
Preview:
Is NIV the answer?
While mechanical ventilation and intubation is often necessary for the sickest, most compromised patients, NIV offers some advantages, especially in these patient populations. For children who are still able to breathe spontaneously, NIV modalities like HFNC allow them to continue breathing on their own schedule with added support, avoiding the issue of ventilator asynchrony and preserving respiratory strength ideally to either delay intubation or prevent it altogether.
Support Strategies and CO2 Visibility
The drawbacks of NIV come back to the control of and visibility into patient status, as discussed above.
Across ventilation modalities, from supplemental oxygen to intubation, clinicians have access to vital signs like SpO2, pulse and respiratory rates, and patient work of breathing. However, visibility to other important parameters (and tools utilized to get it) can vary, depending on how the patient is supported. CO2 is one of these critical values. CO2 monitoring is integral to understanding how well or poorly a patient is ventilating, particularly because…
Meet the tCOM+
Developed with care, designed for confidence.
The tCOM+ offers continuous monitoring of tcPCO2, SpO2, and PR with a sleek new look and feel. This latest model includes significant software advances that improve workflow for providers, while continuing to support reduced blood draws and proactive ventilator management across care areas.

Stay up-to-date with Sentec