MENU
Sentec Article
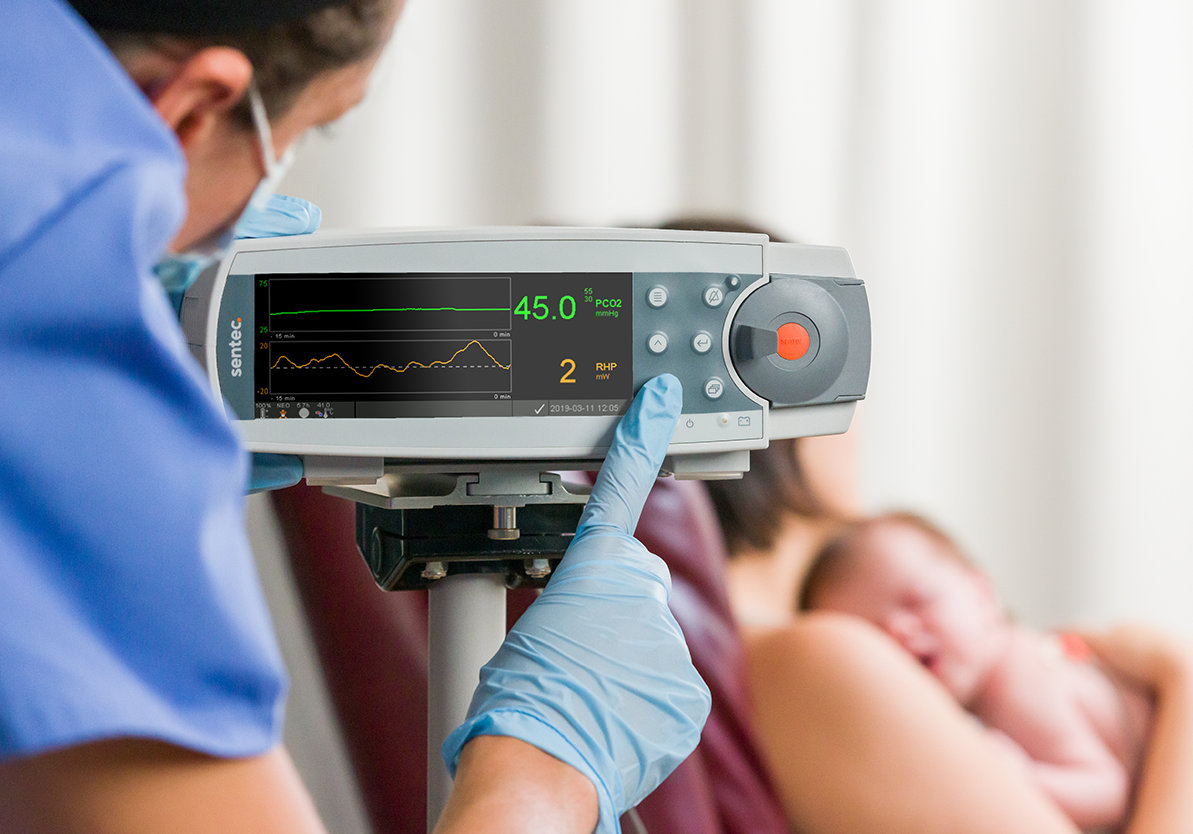
5 Ways End-Tidal CO2 Monitoring Can Fall Short in the NICU
In the NICU, closely monitoring carbon dioxide (CO2) levels is a crucial aspect of care for premature and critically ill infants — fluctuations in CO2 levels can disrupt cerebral blood flow, increasing the risk of intraventricular hemorrhage (IVH), periventricular leukomalacia (PVL), and other cerebral injuries.¹
Guest Article
Transcutaneous CO2 Monitoring in Pediatric Sleep Studies: Case Studies from Nemours Children’s Hospital
In the Pediatric Sleep Center at Nemours Children’s Hospital, transcutaneous CO2 monitoring is a valuable tool that we use for both routine and complex cases.
Sentec Article
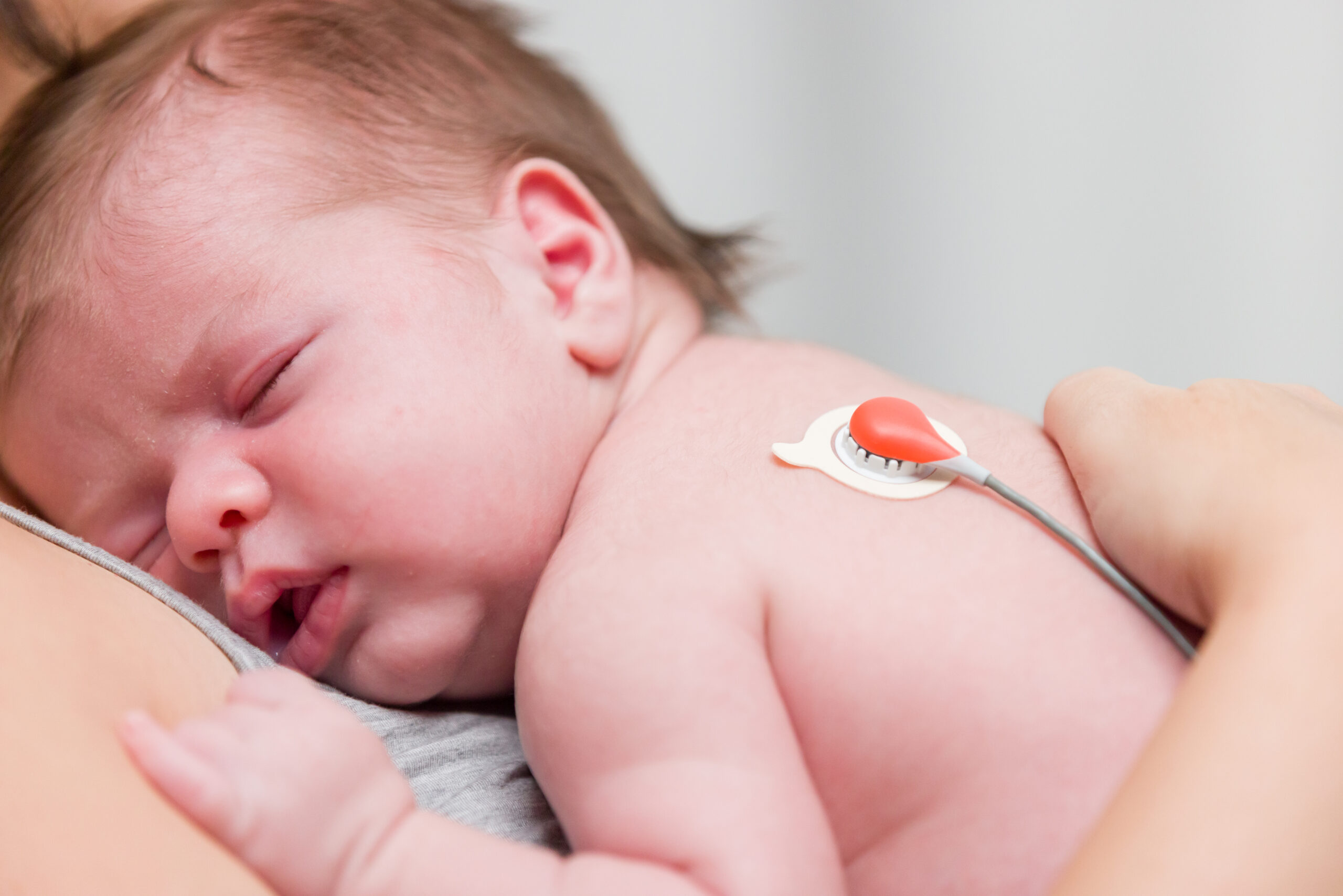
5 Reasons to Consider Transcutaneous CO2 Monitoring for Your Small Baby Unit
In a small baby unit, transcutaneous CO2 monitoring can support care teams in delivering the high level of care preterm babies require. The technology provides continuous CO2 monitoring, supporting timely assessments of respiratory status to aid in protecting the vulnerable brains and lungs of neonatal patients.
Sentec Article
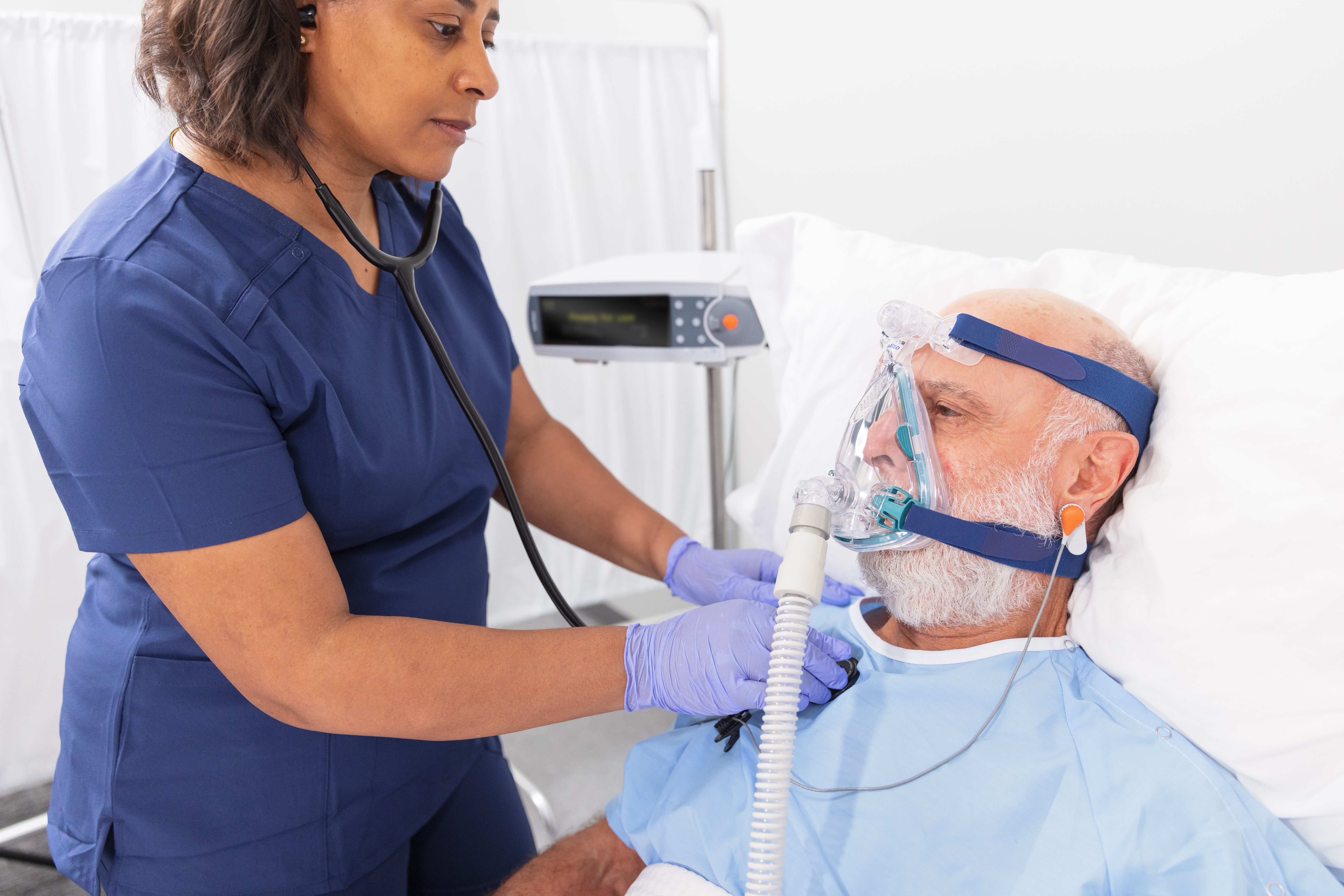
Targeting CO2 to Improve Outcomes in Patients with Chronic Hypercapnia
A growing body of research raises an important question: Are patients with chronic hypercapnic respiratory failure being adequately managed? For these individuals, the presence of elevated CO2 levels alongside normal or near-normal pH levels — a result of renal compensation — is often overlooked.
Patient Story
Stella’s IPV Therapy Story
Diagnosed with spinal muscular atrophy shortly after birth, Stella relies on intrapulmonary percussive ventilation (IPV) therapy as a key part of her daily routine. By offering a proactive approach to her at-home respiratory care, IPV therapy empowers Stella and her family to embrace an active and fulfilling lifestyle with confidence.
Sentec Article
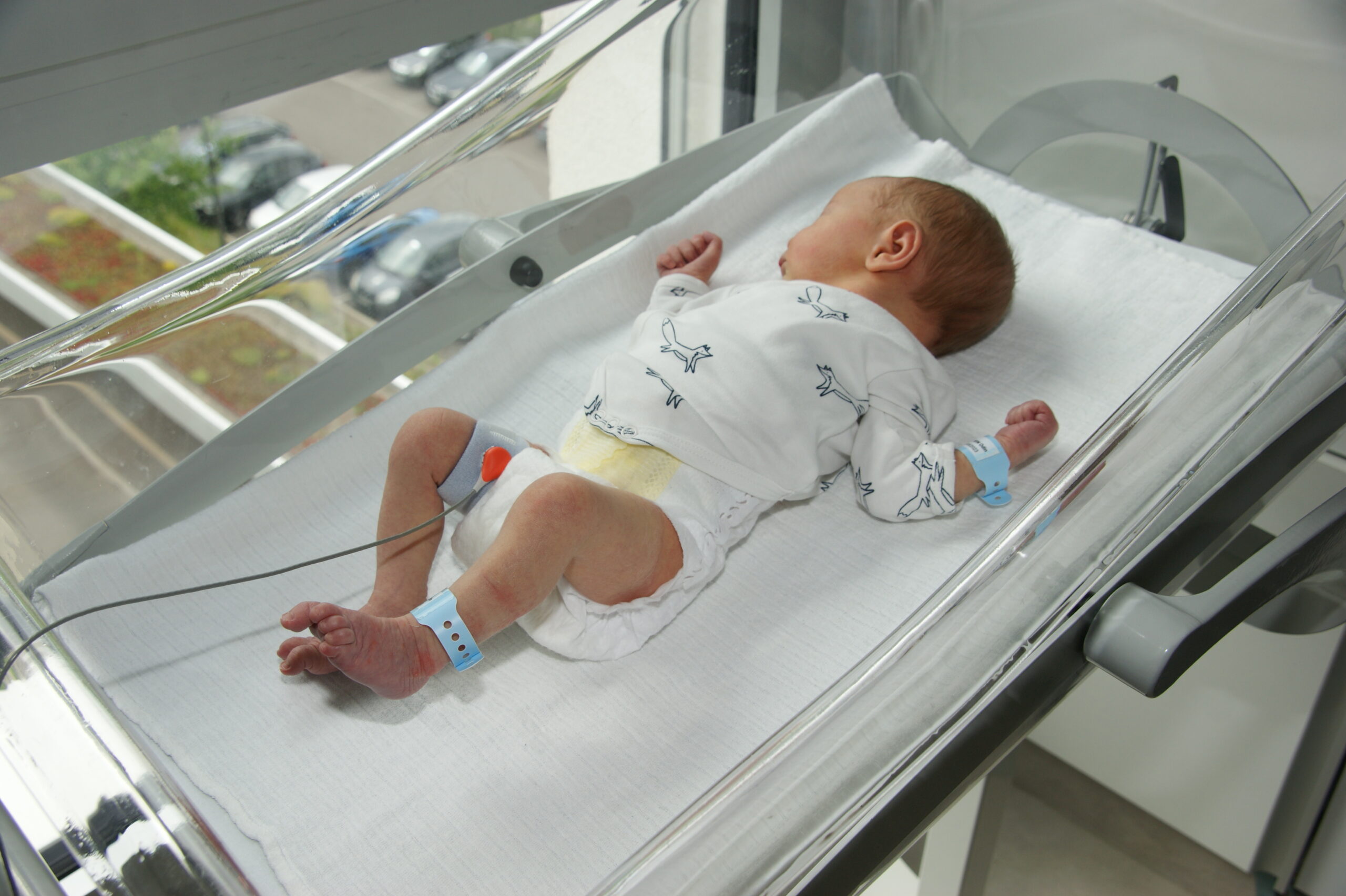
Transcutaneous CO2 Monitoring in the NICU: 4 Clinical Use Cases
In the NICU, critically ill and premature babies receive specialized, around-the-clock care to support their fragile health. This often means using respiratory support to help with their breathing, especially important for little ones with underdeveloped or compromised lungs. By using transcutaneous CO2 monitoring, NICU teams can keep a constant eye on their status, which helps them fine-tune and optimize the support they need.
Sentec Article
How to Get Started with Transcutaneous Monitoring in the NICU
Introducing any new technology in a clinical setting can be an exciting time – you’re eager to use your new tool and see the benefits for patients – especially in the NICU where the smallest, sickest babies are.
Product Spotlight
10 Reasons To Choose Sentec tcPCO2 Monitoring For Your Sleep Lab
With product features designed for the sleep lab, the Sentec Transcutaneous Monitoring System combines ease of use and patient comfort with accurate values regardless of ventilation method or ventilation perfusion (V/Q) mismatch.
Whitepaper
The Downsides & Limitations of Neonatal Blood Sampling
In neonatal intensive care units (NICUs), blood sampling, including arterial blood gas (ABG) tests and capillary blood tests (commonly known as a ‘heel stick’), plays an important role in patient monitoring. These tests help care teams monitor a variety of parameters, including blood pH levels and concentrations of vital gases like carbon dioxide (CO2) and oxygen (O2).
Sentec Article
How Often Should PCO2 Be Monitored in Chronic Hypercapnic Patients? Are Current Practices Enough?
Chronic hypercapnia, characterized by elevated levels of CO2, poses a significant challenge for individuals with conditions like chronic obstructive pulmonary disease (COPD), neuromuscular disorders (NMD), and obesity. Although the negative effects of chronic hypercapnia are widely acknowledged, researchers at the University of Michigan are shedding light on the true urgency of its management.