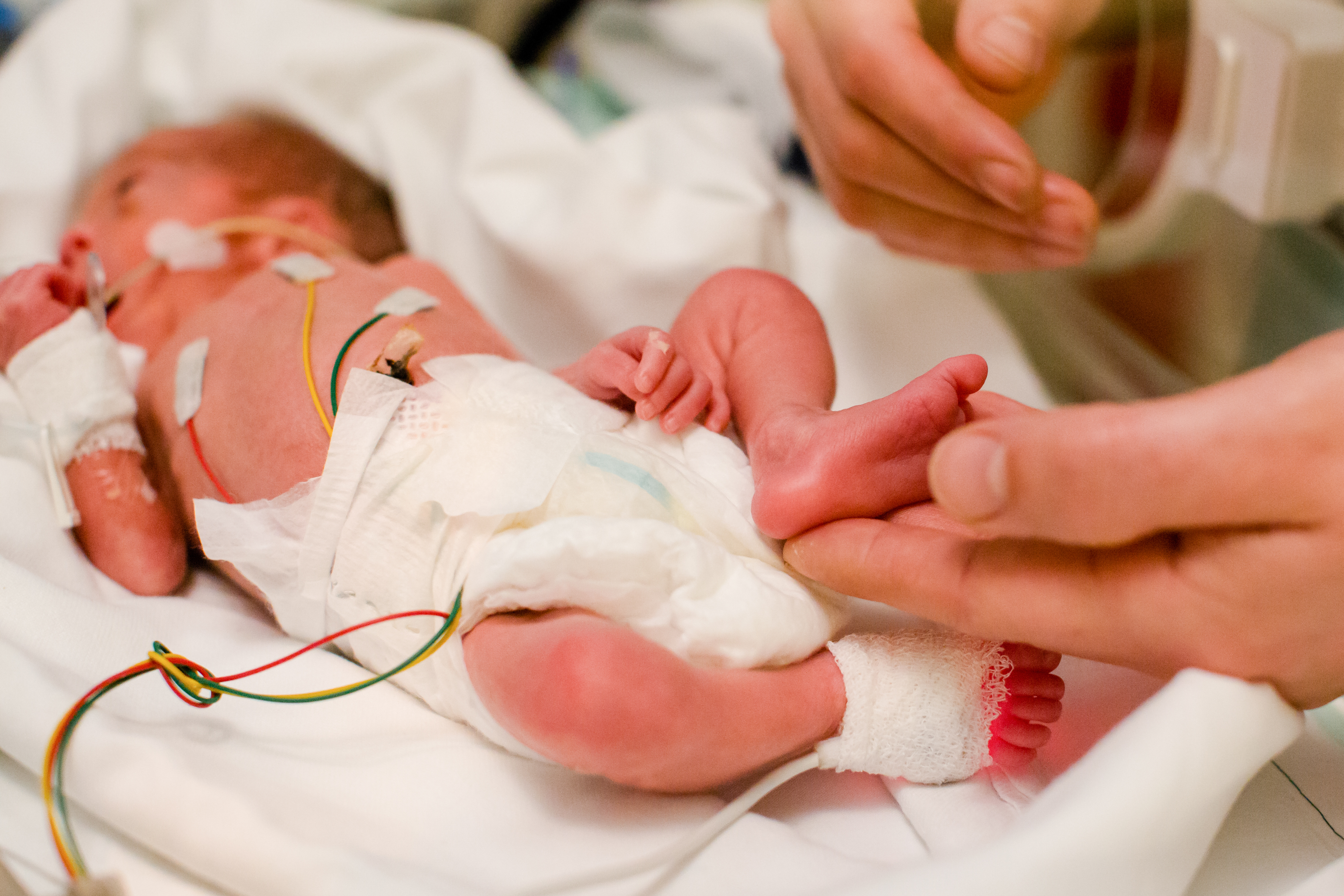
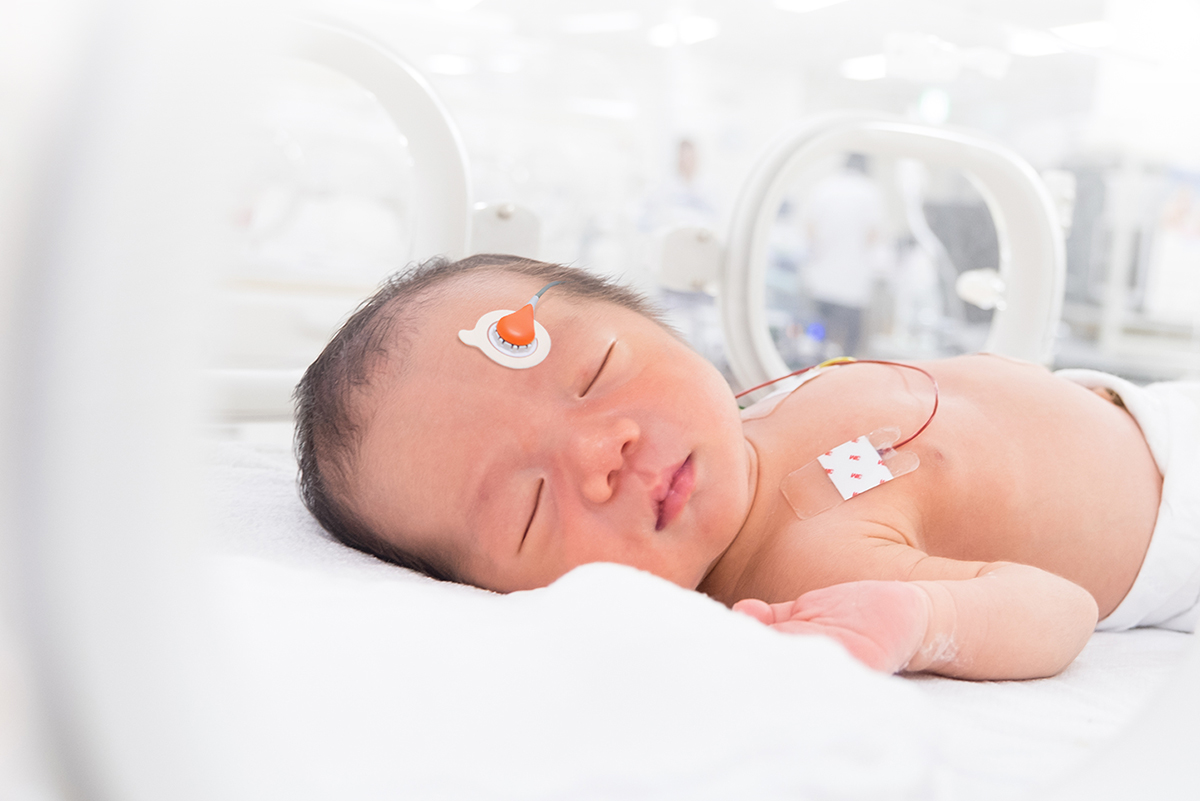
How can transcutaneous CO2 monitoring support your sleep lab?
Sentec transcutaneous technology overcomes limits of pulse oximetry, arterial blood draws and capnography with continuous CO2 monitoring that combines ease of use and patient comfort, with accurate values regardless of ventilation method or ventilation/perfusion (V/Q) mismatch, and product features designed for sleep care settings.
This paper explores the clinical utility of transcutaneous monitoring in the sleep lab as highlighted in the literature, covering:
How can transcutaneous CO2 monitoring support your sleep lab?
Sentec transcutaneous technology overcomes many of the current limitations and challenges associated with CO2 measurement in the NICU by providing accurate, continuous, noninvasive CO2 values regardless of ventilation method or V/Q mismatch. Sentec transcutaneous monitoring provides consistent, independent CO2 measurement all while promoting neuroprotective efforts to deliver clustered care, protect skin integrity, and reduce the frequency of blood draws.
This paper explores the clinical utility of transcutaneous monitoring in the sleep lab as highlighted in the literature, covering:
Meet the tCOM+
Developed with care, designed for confidence.
The tCOM+ offers continuous monitoring of tcPCO2, SpO2, and PR with a sleek new look and feel. This latest model includes significant software advances that improve workflow for providers, while continuing to support reduced blood draws and proactive ventilator management across care areas.

Stay up-to-date with Sentec