Summary
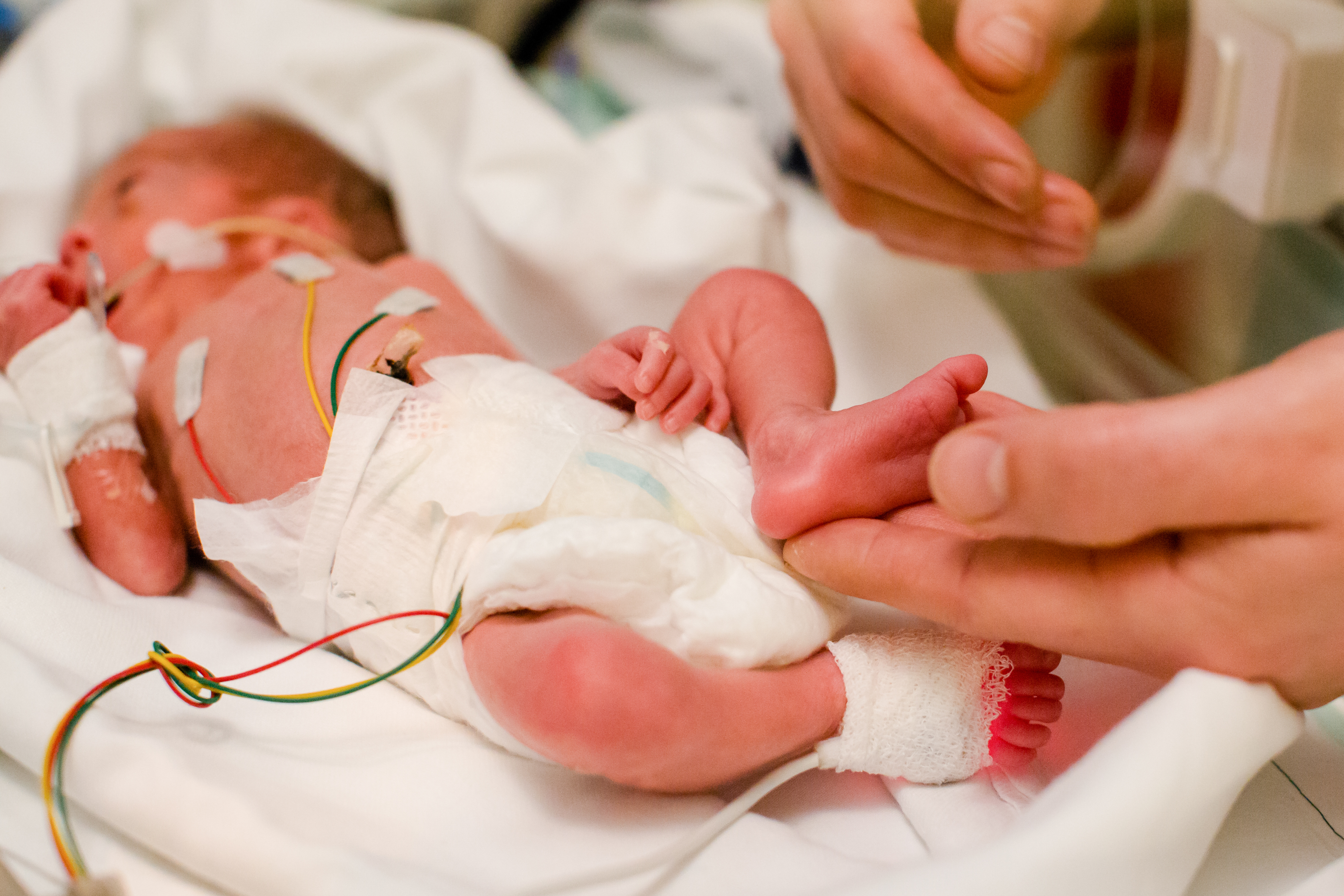
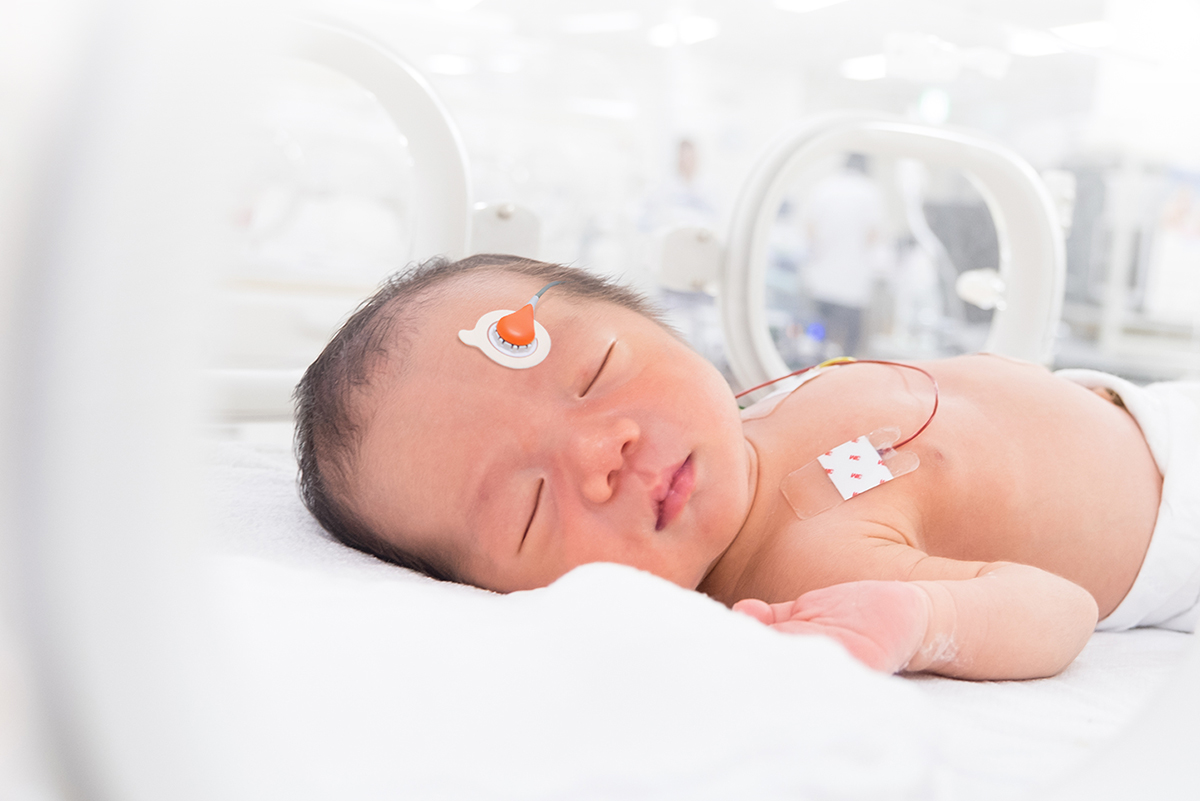
Elevated CO2 levels are common among sleep lab patients, with research indicating that as many as 46% of pediatric patients with sleep-disordered breathing experience a nocturnal change in CO2 of more than 10 mmHg.¹
Lisa DeGuzman, RRT-NPS, RPSGT, CCSH discusses the role of transcutaneous CO2 monitoring in the Nemours Children’s Hospital Pediatric Sleep Center, highlighting its applications in detecting and guiding the management of sleep-disordered breathing among the pediatric population. In this adapted version of her webinar, you can explore the key takeaways and gain insights from the Nemours sleep lab.
1. Pautrat, J., et al. Carbon Dioxide Levels During Polygraphy in Children with Sleep-Disordered Breathing. Sleep Breath. 2015.
Highlights
Summary
Elevated CO2 levels are common among sleep lab patients, with research indicating that as many as 46% of pediatric patients with sleep-disordered breathing experience a nocturnal change in CO2 of more than 10 mmHg.¹
Lisa DeGuzman, RRT-NPS, RPSGT, CCSH discusses the role of transcutaneous CO2 monitoring in the Nemours Children’s Hospital Pediatric Sleep Center, highlighting its applications in detecting and guiding the management of sleep-disordered breathing among the pediatric population. In this adapted version of her webinar, you can explore the key takeaways and gain insights from the Nemours sleep lab.
Highlights

Meet the Author
Lisa DeGuzman, RRT-NPS, RPSGT, CCSH
Pediatric Sleep Center & Pulmonary Function Test (PFT) Lab Manager at Nemours Children’s Hospital in Orlando, Florida
With 37 years in healthcare, Lisa has devoted nearly her entire career to neonatal and pediatric medicine. She spent 15 years as a neonatal respiratory therapist at Arnold Palmer Hospital for Children and Women before moving to pediatric sleep medicine at Nemours Children’s Health. After nine years as a scoring technologist, she assumed a leadership role in 2014. Lisa and her team at Nemours are dedicated to providing sleep study services for a diverse pediatric population, handling everything from routine cases to complex ventilator titrations.
Meet the Author
Lisa DeGuzman, RRT-NPS, RPSGT, CCSH
Pediatric Sleep Center & Pulmonary Function Test (PFT) Lab Manager at Nemours Children’s Hospital in Orlando, Florida
With 37 years in healthcare, Lisa has devoted nearly her entire career to neonatal and pediatric medicine. She spent 15 years as a neonatal respiratory therapist at Arnold Palmer Hospital for Children and Women before moving to pediatric sleep medicine at Nemours Children’s Health. After nine years as a scoring technologist, she assumed a leadership role in 2014. Lisa and her team at Nemours are dedicated to providing sleep study services for a diverse pediatric population, handling everything from routine cases to complex ventilator titrations.

Other resources we think you’ll like
On-Demand CE Webinar: Noninvasive CO2 Monitoring in Sleep Diagnostics
Margie White, BS, RRT-NPS, discusses the role of CO2 monitoring in the sleep lab, the pros and cons of common CO2 monitoring methods, and the benefits of transcutaneous monitoring within this context. Earn credits through AARC and AAST.
Other resources we think you’ll like
On-Demand CE Webinar: Noninvasive CO2 Monitoring in Sleep Diagnostics
Margie White, BS, RRT-NPS, discusses the role of CO2 monitoring in the sleep lab, the pros and cons of common CO2 monitoring methods, and the benefits of transcutaneous monitoring within this context. Earn credits through AARC and AAST.